One of my favorite topics, because it’s so mundane, & yet there are so many interesting subtleties about diagnosis, that so many seasoned clinicians fail to appreciate. I could go on ad nauseum about pharyngitis (but will try to contain my enthusiasm a bit).
A patient presents with “sore throat” of 2-days’ duration. It’s probably a benign virus, but might be Strep (Streptococcus pyogenes, aka Group-A beta-Hemolytic Streptococcus or “GABHS” for short). Both are self-limiting — viruses can’t be treated, Strep resolves so soon it’s debatable if penicillin (even in the first 24 hours) helps hasten this. Shouldn’t our receptionist advise the patient to save time and money and just go home?
Maybe. But for one, some life-threatening diseases can present with sore throat:
** Deep Mouth & Throat Infections — These include Epiglottitis, Retropharyngeal Abscess, Peritonsillar Abscess, Ludwig’s Angina, Lemierre syndrome (thrombophlebitis of the internal jugular) & others. Nothing subtle — patients are febrile & obviously ill. Often, they can’t even open their mouth (trismus), or have big swollen necks. If they’re bent forward drooling, or you auscultate stridor at the trachea, don’t attempt further exam, lest it provoke complete airway obstruction. Call 9-1-1 and ship to E.D.
** Early Peritonsillar Abscess (PTA) — I think of this a couple of times a year. Patients are febrile, and just feel pretty bad, with a sore throat.
Every time you examine a “sore throat,” look for the 2 telltale signs of a PTA:
- Deviation of the uvula away from the abscess
- Swelling of the soft palate (which may hide the actual tonsil)


“Deviation of uvula” means the base of the uvula, not the tip. There are lots of cheesy variations in normal uvulas:


ENT’s may say that PTA’s all need I&D’s, but I’ve given high-dose penicillin or clindamycin to fairly uncomfortable febrile patients able to open their mouths enough to detect these signs, & they’ve done well. Causative organism may be either Strep or anaerobes.
** Diphtheria — Extremely rare;suspect if you see a coalescing grayish-white membrane, & the patient had recently traveled to the 3rd World or Eastern Europe. Fevers are variable. Dangers are asphyxiation & myocarditis.

** Neutropenia — Causes mucosal & gingival ulcers &/or bullae (worse than the tiny vesicles of Coxsackie Virus “hand-foot-&-mouth disease,” though you can always check the hands & feet). Might be caused by a medication, or frank leukemia. Most rare, but suspicious findings mandate a CBC.
** Acute (Primary) HIV Infection — Up to 80% of people just infected with HIV develop an acute illness 9-30 days later. Almost all have fever and lymphadenopathy, 75% may have a sore throat. The syndrome resembles mononucleosis, and lasts 1 to 3 weeks.
I never used to consider Acute HIV until a sore throat had gone on at least 5 days, by which time both simple viruses and Strep will have resolved on their own. There’s obviously plenty of time to diagnose and treat HIV, and I’d go nuts addressing this for every patient who presents with “sore throat x2 d.” But now I worry more, because our “2-day-ill” patient may present only this one time, and missing self-limited Acute HIV has major consequences:
- An estimated 50% of all HIV transmission is due to Acute HIV, when patients carry enormous levels of circulating virus. This degree of viremia may persist 4 months. So even though the sore throat gets better, people are out and around infecting others.
- If our Acute HIV patient was unlucky enough to have been infected with a drug-resistant viral strain, it’s best identified during primary infection. If they get diagnosed a few years later, the pool of mutated virus may have been replaced by the more competitive drug-sensitive strain. Then a resistance assay will miss the mutation, at that point latent and “archived.” But once the patient starts treatment, eliminating all sensitive viruses, the resistant strain will emerge, develop more resistance, & completely blow the entire medication regimen.
More about Acute HIV later. But even at the very onset of sore throat plus fever, I bring it up & urge certain patients to return if symptoms last a few more days. These cases include:
- Patients with major risk factors for acquiring HIV.
- Presence of “atypical” lymphadenopathy. A “typical” sore throat may cause swollen and tender tonsillar & anterior cervical nodes, but NOT the posterior cervical, occipital, axillary, or epitrochlear.
- A funny rash, maculopapular, often subtle, usually on the trunk (25%).
** Strep Throat — The reason this is “life-threatening” is that it can cause Rheumatic Fever (RF). That’s pretty rare in the US today [in contrast to the 3rd World]. Indeed, the C.D.C. removed RF as a notifiable condition way back in 1994; only six states and Wash DC have maintained mandatory reporting.
Not good, in my mind. For one, incidence of RF may be significant among poor, crowded populations. Also, the progressive decline of RF has been punctuated by unexpected outbreaks, some in middle-class suburban communities. This could be explained by the new entrance of rheumatogenic strains of Strep (though the pathogenesis of RF remains unclear, and the role of specific strains debated).
From a clinical perspective, concern about RF is the primary rationale for caring about Strep Throat (another might be to limit transmission). Acute RF is a disease of kids ages 5-15; no cases occur after 30 [existing RF can relapse at any age]. Back when the disease was more common, a cost-effectiveness analysis concluded it might sometimes be appropriate to simply treat every sore throat (valve repairs plus lifetime anticoagulation get pretty expensive). Conversely, some now argue that RF is so rare, we might simply ignore Strep — don’t test, certainly don’t treat.
Current recommendations suggest testing for Strep when 3-4 of the Centor Criteria are present:
- Fever (or history thereof)
- Presence of Exudate
- Tender anterior cervical nodes (including tonsillar node at angle of jaw)
- Absence of cough and rhinitis
Brief comment about “Exudate” — all that’s white isn’t pus. True “exudate” should appear splotchy and “pasted-on.” If the white stuff fits neatly into a tonsilar “crater,” it’s just old food, etc. stuck in a crypt (scar from prior infection).

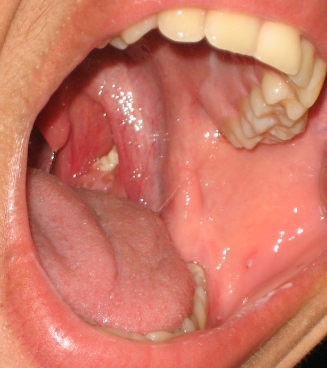
Exudate Not Exudate (Gunk in Crypts)
Not-so-brief comment about Testing. We have 2 methods: 1) Cultures, which take 24-48 hours; and 2) Rapid Tests (by antigen-detection), with results in a few minutes.
Literature used to say the Rapid Tests were only 70% – 80% sensitive compared to the Culture. Most authorities consider current ones at least 95%. So it’s no longer really necessary to obtain two separate swabs (which patients never appreciated), and send for a Culture if the Rapid Test is negative. I stick with the Rapid Test alone. If RF resurges, you’d certainly want to add a culture — treating Strep throat within 9 days of onset prevents RF.
Another rationale for performing a “Throat Culture” is that it might identify Group C or Group G Strep. These may be culprit pathogens, but don’t cause RF. Any other bacteria, e.g. Neisseria meningitides (Meningococcus), is merely a colonizer. The “Throat Culture” costs more than a “Beta-Strep Screen,” which is a actual culture but only seeks to identify presence or absence of GABHS.
Actually, all these methods lack specificity, because 10% to 20% of people are colonized with Strep. They get a viral illness, and their Strep test is thus false-positive! No way to tell, except by the Gold Standard: draw blood for an Antistreptolysin O (ASO) titer. A negative antibody, which converts to positive 3 weeks later, gives absolute proof of recent Strep [by which time the throat’s all better, & RF has begun if it were going to happen].
Swabbing the Throat (a final word): I was taught that proper specimen collection “should draw blood.” Not exactly, but you can’t just blindly wiggle a swab around the back of the mouth. You have to clearly identify each tonsil (or empty fossa if prior tonsillectomy), & rub vigorously! Some pearls for Swabbing Throats:
- Avoid midline, which is where the Gag is provoked.
- Have the patient relax as much as possible, maybe NOT stick the tongue way out.
- If “Say Ah” doesn’t help, have them YAWN. A sustained yawn gives a beautiful clear target, no gag at all.
WRAPPING UP
An adult presents with 1-2 days of “Sore Throat.” They don’t look ill, & we have no reason to suspect Primary HIV infection. Their risk of Rheumatic Fever is very minimal, probably zero if they’re over 30.
- But I ask all sore throat patients if they ever had RF as a child. If so, they get auscultated for murmurs, & empiric penicillin (no testing) if history or exam are convincing for prior carditis. This is especially important for persons who grew up in the Third World.
Some Possible Scenarios:
- Obviously Viral: Cough / runny nose & no throat findings
- No fever or exudate, but some tender nodes & no URI Sx (2/4 Centor Criteria)?
- Fever, exudate, adenopathy, and no URI Sx (4/4 Centor Criteria)?
Experts would say for Scenario #2, we’d still reassure them “It’s just a virus,” and recommend gargles & milk-‘n-honey & ibuprofen or whatever. For #2, you’d do a Rapid Strep Test to base treatment.
I say, do whatever you want. But mull over some considerations:
- If you do a Rapid Strep for Case #1, they may leave more satisfied and reassured, which conveys some therapeutic effect. So why not? Heaven knows, we spend lots more health care dollars in other ways.
- For Case #2, if Rapid Test is negative, might it be false-negative? And they could have Group C or G Strep, which respond to penicillin. Should we simply treat without testing?
- Should we do a more sensitive culture, and start treatment 1-2 days later, when symptoms have already resolved?
- Should we educate our adult patients that nobody needs diagnostics or treatment for 1-2 days of sore throat anyway (“Next time, don’t even bother us”)?
Personally, I tend to opt for the top consideration above, but will probably get dinged by auditors at some point.
Can we conclude that this whole discussion was a waste of time? Not really, because we see lots of sore throats, and need a good grasp of the subtleties. And for Pediatrics, be less nihilistic & order Rapid Strep Tests.
Next time, our sore throat will have gone on 4-5 days [see Sore Throat – 2].
Hello there:)
I am a primary pnp student and this site is really informative. I am so glad that you have posted pictures along with prescriptions. Sometimes prescription only is vague.
Thank you so much for your awesome posts!
Stupid auto correction! It should be “description” not prescription!.lol
Also, Can’t see the picture under diphtheria (I am using Chrome)
1
1′”
1����%2527%2522